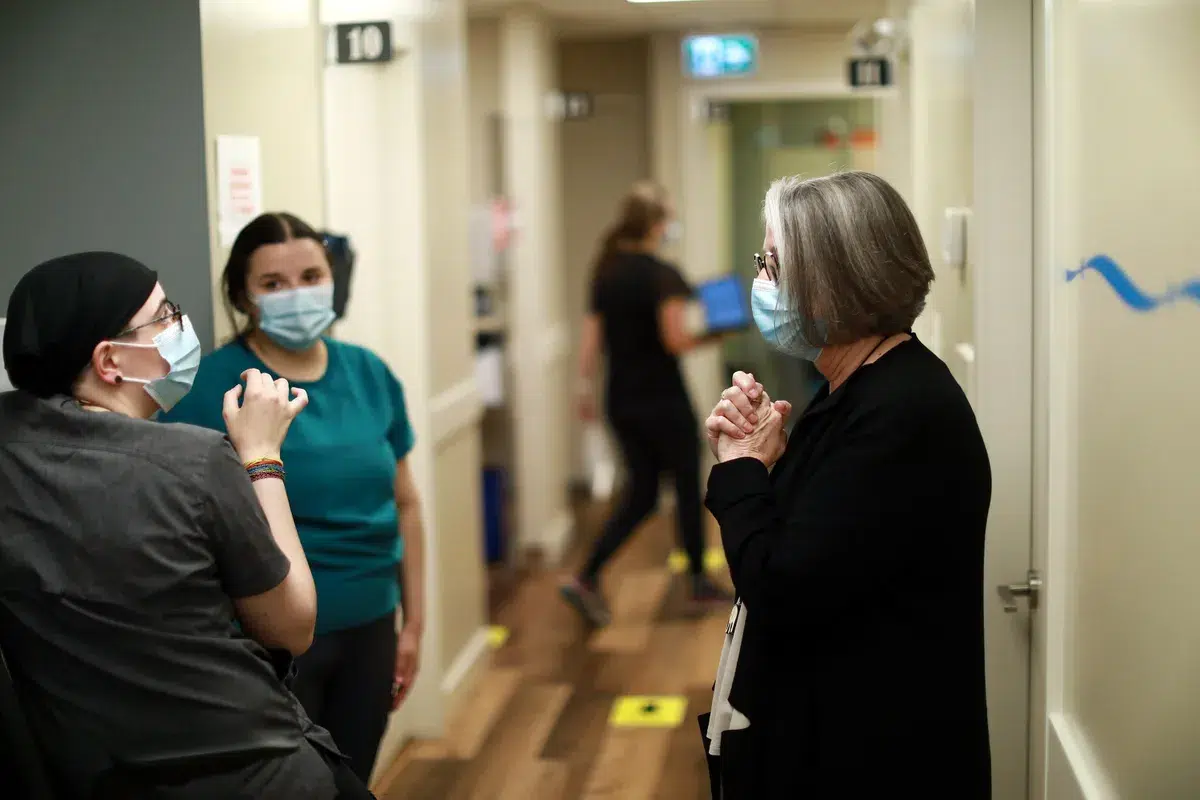
Originally published in The Globe and Mail, written by Karen Howlett. Photos by Chad Hipolito.
Karen Morgan had a bird’s-eye view of a looming exodus of family doctors long before the crisis hit her tiny community in British Columbia – and the rest of Canada.
In the early 2000s, doctors on the Saanich Peninsula, on the southeast coast of Vancouver Island, were starting to retire, and nobody was coming in to replace them.
“Most of the doctors were of the same generation,” said Ms. Morgan, then the executive director of the Saanich Peninsula Hospital & Healthcare Foundation. “They’d all come out to B.C. in the late sixties, early seventies. And they were all retiring around the same time.”
With the help of the hospital foundation, the community raised money from local residents to open two medical clinics to ensure more people had a family doctor – an initiative that took 12 years to complete. The first Shoreline Medical clinic opened in the town of Sidney in September, 2016; today, Shoreline has two clinics with 24 doctors.
How the Saanich Peninsula responded to its shortage of family doctors can be replicated in other communities across Canada, advocates say. The Shoreline clinics serve as examples of a grassroots response to a problem left largely unaddressed at the provincial and federal levels. A recent Globe and Mail article found significant gaps in data on where and how family doctors work. These gaps mean Canadians don’t know the true capacity of primary care in the country, hindering the provinces’ ability to deal with a growing crisis.
“I think we’ve got to do a little more ourselves,” said Dale Henley, co-chair of Shoreline Medical Society, the non-profit that owns and operates the clinics, and a former board member of the hospital foundation. “We can’t just keep looking at governments all the time, because they’re not that good at it.”
The Saanich Peninsula has not solved its shortage of doctors altogether. There are still 10,000 people in a community of 60,000 who don’t have a family doctor. But at a time when access to primary care is getting worse in many parts of the country, including Vancouver Island, the situation in the community has remained stable since the first Shoreline clinic opened.

CHAD HIPOLITO/THE GLOBE AND MAIL
It took several years to transform the vision for a medical clinic into reality.
In 2004, Ms. Morgan began sounding warning bells about the pending retirement of local doctors and how that could potentially cripple health care in the community, as well as the Saanich Peninsula Hospital.
The peninsula was originally a small farming and fishing enclave, and its hospital operates under a rural model, in which family doctors also care for hospital patients. Unlike hospitals in larger communities in B.C., it does not have its own doctors on staff to look after acute-care patients.
Together with doctors, Ms. Morgan began working on plans in 2005 for the first clinic. She said the traditional way of providing primary care, in which older doctors practised alone, seeing patients from infancy to old age, was not appealing to their younger peers. She looked at other provinces, including Ontario, that were experimenting with team-based primary care centres, to help design a collaborative environment in which doctors would practise medicine and others would run the business.
Board members of the hospital foundation were initially reluctant to earmark funds raised from donors for the clinic, Mr. Henley said. They were more accustomed to using the money to buy new equipment for the hospital.
By 2013, the peninsula was in a “crisis situation,” with many doctors within two years of retirement, said Ms. Morgan, Shoreline’s interim executive director. Mr. Henley, a lawyer and long-time resident of the retirement community of Sidney, was the first board member to endorse plans for the clinic, she said.
The shortage of family doctors persuaded him that the foundation had to look beyond the hospital’s four walls, Mr. Henley said. “Our average donor might like to have a new MRI [for the hospital]. I think they’d rather have a family doctor if they had a choice.”
Along with donations to the hospital foundation, Sidney’s municipal government also pitched in, Mr. Henley said, providing Shoreline Medical with a bridge loan of $190,000.

CHAD HIPOLITO/THE GLOBE AND MAIL
When the clinic in Sidney opened its doors six years ago, Christopher Dowler, its medical director, was among the first four family doctors to join. Treating patients in the community and the hospital allows him and his colleagues to provide more effective care, he said.
“We know our patients. We are there for them when they’re sick and when they’re well, regardless of the setting.”
The clinic attracts younger doctors, he said, because of the support they get both clinically, from their peers, as well as administratively. The hospital foundation helps cover some of the clinic’s overhead costs.
It has 13 family doctors and also operates the only walk-in clinic on the peninsula for people who don’t have their own doctor.
Dr. Dowler is optimistic that a new payment model for family doctors in B.C., unveiled Oct. 31, will help the clinic recruit even more doctors. The existing fee-for-service model, which has not kept pace with the way doctors practise, is a key reason why working in primary care has become less attractive. The new model compensates doctors based on time spent with a patient, the number of patients in a doctor’s practice and their medical complexity.
“It’s a huge step in the right direction,” Dr. Dowler said. “It will help physicians with existing practices justify staying in the profession.”